FDNY Pro EMS: Commissioner’s Brief for 1/2016
March 1, 2016
Preparing for Success: The What Ifs
March 1, 2016The best and safest strategy for treating a patient suspected of having any communicable disease, but particularly Ebola Virus Disease (EVD), is:
- Assure early identification of the infected patient.
- Assure proper use of personal protective equipment (PPE).
- Assure proper cleaning and decontamination.
Patient Identification
In New York City, during the Ebola crisis, FDNY was on high alert for patients possibly having the disease who had (1) fever and/or any of the symptoms considered to be the telltale signs of EVD and (2) traveled recently to one of the West African countries affected by EVD outbreak within 30 days prior to the onset of symptoms.
Of course, it was possible that a patient could have been found to be suffering from symptoms consistent with EVD and recent travel to an index country, but did not get assigned an FT call type by the responding EMTs or Medics. Keep in mind, no matter how conscientious our ARDs, the call type is dependent upon the caller’s answers, which are not always accurate. Therefore, all providers were told to make a three-foot assessment of a patient before making physical contact, while simultaneously asking the patient and family questions regarding symptoms and travel history.
If symptoms and travel history suggest EVD, the crew shall maintain a safe distance of at least three feet and request the appropriate resources to respond, based on patient stability.
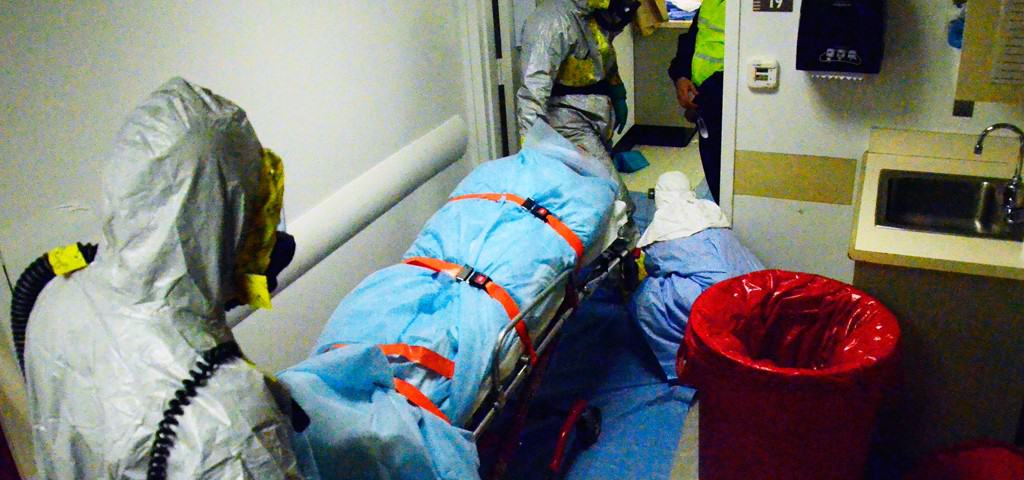
Proper PPE
During the EVD outbreak, if a patient was coughing, members were advised to have the patient wear a surgical mask to limit droplet transmission.
Fit-tested respirators and eye protection (goggles or face shields), PPE/bunker-style pants and gowns always should be worn by EMS personnel performing any aerosol-generating procedures on patients with febrile respiratory illness. This is a best practice for all communicable diseases.
Aerosol-generating procedures include nebulized treatments, intubation, tracheal suctioning and laryngoscopy. Administration of nebulized (aerosolized) medications (e.g., Albuterol) may be done only via a nebulizer with a one-way valve (e.g., Aeroeclipse II Breath Actuated Nebulizer) or via a disposable, metered-dose inhaler (MDI) with spacer.
Cleaning and Decontamination
Decontamination of personnel and ambulance is critical. All disposable materials should be left at the destination hospital whenever possible. All non-disposable equipment used in the treatment of the patient should be cleaned in accordance with normal decontamination procedures.
Infection control procedures should be undertaken, including aggressive hand washing with soap and water as soon as possible, which is essential in limiting disease transmission. And, as always, responders should wear full PPE when cleaning non-disposable equipment.
In closing, always remember these common sense steps to protect yourself from contamination:
- Keep hands away from face.
- Limit surfaces touched (similar to crime scene operations).
- Change gloves when torn or heavily contaminated.
- Perform hand hygiene.
About the Author
Dr. Bradley Kaufman, MD, MPH, FACEP, is the First Deputy Medical Director for the FDNY, and is the Medical Director for Emergency Medical Dispatch and the EMS Bureau of Training. He serves as a Medical Manager with FEMA’s New York Task Force 1 USAR team. He is Board Certified in both Emergency Medicine and EMS Medicine, is an Associate Professor of Emergency Medicine at the Hofstra Northwell School of Medicine, and an Attending Physician at the Northwell LIJ Medical Center.
Read More from Pro EMS 1st/2016